TL;DR
- AI in post-acute care is solving operational problems first (referral intake, insurance verification, and portfolio-level reporting), not clinical ones. The facilities that screen and respond to referrals fastest win the most admits, and AI compresses what was a 40+ minute manual review into minutes.
- The results are already measurable. One four-facility operator reported an estimated $800K in additional billable revenue within 60 days. A 50-facility operator saw a 45% reduction in review time and 2x intake capacity without adding headcount. Pearl Healthcare, a 14-facility operator, saw a 43% census increase in their second quarter after switching to AI-powered intake.
- The biggest unlock for multi-facility operators isn’t speed, it’s centralization and structured data. AI-powered intake captures referral volume, decline reasons, response times, conversion rates, and payer mix across every building, turning intake from a reactive function into a strategic one.
If you work in post-acute care, you’ve heard the pitch: AI is going to transform healthcare. And if you’ve been in this industry long enough, you’ve probably developed a healthy immunity to the latest technology that’s going to save the day.
Indeed, most of the AI conversation in healthcare is devoted to acute care. AI in post-acute care barely registers. And when it does, the coverage tends to be vague: AI will “personalize treatment” and “optimize resource allocation.” That’s dramatically unhelpful for someone running admissions across 12 skilled nursing facilities with a team that’s already stretched thin.
Meanwhile, the pressure your team actually feels every day looks nothing like the headlines:
- Staffing shortages aren’t theoretical; they’re the reason your intake coordinator is reviewing 40 referrals a day while toggling between four different portals
- Margins are tight enough that one admissions mistake can wipe out a month of gains
- The systems that are supposed to hold everything together (referral portals, EHRs, fax machines, email threads) don’t talk to each other
These are the real problems AI needs to solve in post-acute care.
Why post-acute care is different (and why most AI conversations miss the point)
Post-acute care is fundamentally an operational coordination problem. The challenge is how do you move a patient from a hospital referral to the right facility, with the right clinical fit, the right insurance coverage, and the right documentation, quickly enough to win the referral and accurately enough to protect your organization and deliver improved patient outcomes?
At most facilities, that process still looks like this:
- A referral comes in through one of several portals (or by fax, or by email)
- An intake team member opens a clinical packet (often 100 pages or more) and starts the manual review
- They check diagnoses against facility capabilities, looking for clinical red flags, verifying insurance eligibility, running sex offender checks, cross-referencing medication lists, and assessing whether the facility can actually serve this patient.
On a good day, that takes roughly 40 minutes. On a busy day, it takes longer, or it doesn’t happen at all, and the referral goes to a competitor. But that timeline is the single biggest driver of census growth or census loss. Put directly: the facility that says yes fastest, wins.
And here’s where the challenge balloons: multiply that process across 10, 20, or 50+ facilities. Then add:
- The fact that referrals might be going directly to individual buildings instead of through a central intake team
- Inconsistent human analysis; one admissions director applies different criteria than another
- The reality that when central intake approves a patient and sends the information to a facility, the facility often re-reviews the entire packet from scratch because no clinical summary was passed along
This is the actual problem that AI needs to fix first: the core, unglamorous, high-volume work of getting the right patients into the right facilities without burning out your team or losing revenue to slower decisions.
Where AI is delivering measurable results in post-acute care today
The good news: AI tools (including ExaCare AI) already solve specific, high-value problems in post-acute operations. One four-facility operator reported an estimated $800K in additional billable revenue within 60 days of implementation. Here are three areas where the results are real:
1. Referral intake, admissions screening, and centralized referral management
AI-powered admissions screening uses natural language processing to ingest the full referral packet, reading and extracting the financial information, clinical data and patient history that matters, and applying facility-specific admission rules through a purpose-built AI model to produce a structured summary. What used to take a skilled intake coordinator 40+ minutes of manual review can be compressed to minutes.
But speed is only part of the story: the bigger unlock, especially for multi-facility operators, is consistency and centralization.
| Without AI | With ExaCare AI |
| Intake team manually reviews 100+ page referral packets, taking 40+ minutes per referral | AI reads the full packet in minutes, extracts clinical and financial details, and applies your facility’s admission rules |
| Referrals arrive through multiple portals, fax, and email. Some bypass central intake entirely | All referrals land in one system regardless of source, giving central intake full visibility |
| Each facility may apply different criteria to the same type of referral | Every referral is evaluated against that building’s specific admission rules, applied consistently and systematically every time |
| When central intake approves a patient, the facility re-reviews the packet from scratch | Facilities receive a structured clinical summary with the recommendation, eliminating duplicate work |
Consider what happened at a 50-facility post-acute operator. Before adopting ExaCare AI’s AI-powered intake, their referral process was, in their VP of Growth’s words, “the wild west.” Referrals arrived through multiple portals and sometimes went directly to individual buildings, bypassing central intake entirely. Up to 20% of referral volume had no centralized visibility. Each review took 40+ minutes, and when central intake passed a patient to a facility, the building would start the same manual review process over again from scratch.
After implementing ExaCare AI’s AI-powered admissions system as the operating system for centralized intake, this organization saw:
- 45% reduction in average referral review time, with 89% of referrals reviewed in under 22 minutes
- 60% increase in monthly referral volume, not because more referrals existed, but because centralizing all referrals into one system meant they were finally capturing and tracking the full universe
- 2x intake capacity for their central team, without adding headcount
The Director of Central Intake put it simply: the system took subjective feelings out of the referral decision and turned it into a consistent matrix. Every referral, across all 50 buildings, evaluated against the proper criteria, at the same standard.
2. Insurance verification, reimbursement accuracy, and acuity leveling
At the most basic level, AI automates insurance verification:
- Checking coverage
- Confirming co-pay days
- Determining SNF eligibility before a patient is admitted
The manual alternative (phone calls to insurers, toggling between payer portals, relying on intake staff or healthcare professionals to catch financial red flags buried in dense documentation) is the kind of work that generates expensive mistakes when your team is handling 30 verifications a day and the phone hold times alone eat half the morning.
Insurance verification is the floor. The even bigger financial opportunity is in what happens next: pre-authorization and acuity leveling. Here’s the problem that solves: when a skilled nursing facility admits a patient under a Managed Medicare or commercial insurance plan, the facility needs to secure authorization at the right reimbursement level. In practice, the process of interpreting payer contracts, pulling the right clinical documentation, and justifying the appropriate level is manual, time-consuming, and often results in facilities getting authorized at a lower level than the patient’s acuity warrants.
That’s money left on the table with every admit.
AI is now being applied to this workflow directly: ingesting payer contracts and referral documents, analyzing the clinical documentation to determine the appropriate level of care, and generating authorization requests with in-line clinical citations to support the recommended level.
| Without AI | With ExaCare AI |
| Staff call insurers, toggle between payer portals, and manually verify eligibility, often under time pressure with 30+ verifications a day | Coverage, co-pay days, and SNF eligibility are checked automatically before admission |
| Pre-auth prep requires an hour of pulling clinical documentation, interpreting payer contracts, and assembling justification, per patient | AI ingests contracts and referral documents, determines appropriate acuity level, and generates authorization requests with in-line clinical citations |
| Facilities frequently get authorized at lower reimbursement levels than the patient’s acuity warrants | Early deployments show higher reimbursement on 40% of managed care days vs. 11% baseline, an estimated $385K per facility annually |
| MDS coordinators and case managers spend hours on paperwork instead of patient care | Pre-auth prep drops from ~1 hour to minutes, freeing clinical staff for direct care |
The time savings compound the financial impact. Pre-authorization prep that previously took clinical staff an hour per patient can be reduced to minutes, freeing MDS coordinators and case managers to focus on direct patient care rather than document assembly and contract interpretation.
For operators navigating increasingly complex payer mixes (especially those with growing Medicare Advantage populations), automated verification and acuity leveling isn’t a nice-to-have, it’s a revenue protection function.
3. Data, AI, and portfolio-level intelligence
I’ve watched operators sit in quarterly reviews trying to explain why census dipped, armed with nothing but gut feel and a spreadsheet someone pulled together with data from numerous platforms. When your referral data is structured and centralized, those conversations change completely. You can see exactly where referrals are stalling, which buildings are leaving admits on the table, and whether your payer mix is shifting under your feet.
This matters because the questions that drive growth in a multi-facility organization aren’t about individual referrals. There are questions like:
- Why are we declining referrals at Building 7 at twice the rate of Building 12? Is it a clinical capability gap, a staffing issue, or an overly conservative admissions director?
- Which hospitals are sending us the most referrals, and what’s our win rate from each source?
- Is our payer mix shifting? Are we seeing more Managed Medicare and less traditional Medicare, and what does that mean for revenue?
- Where are we slow to respond, and is that costing us admits?
These are strategic questions. Without structured data, answering them requires manual audits, spreadsheet exercises, and guesswork. With AI-powered intake generating structured data on every referral, the answers are available in real time.
| Without AI | With ExaCare AI |
| No record of why referrals were declined, how long response took, or what payer mix looks like across buildings | Every referral generates structured data: decline reasons, response times, conversion rates, payer mix, and source performance |
| Leadership relies on gut feel and manually assembled spreadsheets for quarterly reviews | Real-time dashboards show exactly where referrals are stalling, which buildings are underperforming, and how payer mix is shifting |
| No way to compare performance across facilities on the same metrics | Portfolio-wide visibility lets you benchmark Building 7 against Building 12 on the same criteria |
| Intake is a reactive function: Process referrals as fast as you can | Intake becomes a strategic function: referral data informs capacity planning, service line expansion, and hospital relationship management |
This is the shift from reactive intake (“process referrals as fast as you can“) to strategic intake: Using referral data to inform capacity planning, service line expansion, payer strategy, and hospital relationship management.
Making it real: Pearl Healthcare
Pearl Healthcare, a 14-facility operator in the Chicago area and ExaCare AI customer since April 2025, runs a decentralized model. Each building has its own admissions director, with regional oversight from leadership. Their previous CRM was unreliable. System outages, broken referral platform integrations, and reporting accuracy that leadership couldn’t trust. Referral communication was buried in emails across 14 buildings, and regional directors had no consistent way to see what was happening at the facility level. After switching to an AI-powered intake system, Pearl saw a 43% increase in census in their second quarter, which leadership attributed directly to operational efficiency gains (not marketing changes or new staff). Their referral-to-admit win rate increased 2.6x, and 76% of referrals now have a first review in under 20 minutes, up from 62% before. What Pearl’s VP of Business Development noticed most wasn’t the speed, though. It was that her admissions directors were happier. She got time back for strategic work, like market development, C-suite meetings, and getting out in the field. The system freed leadership from “managing the system”.
Where AI in post-acute care is headed, and what to watch for
The results in intake, financial screening, and portfolio reporting are already there for the taking. What we’re pushing towards now is next level: AI that doesn’t just support the admissions decision, but extends across the full patient workflow.
AI workflows that extend beyond the intake decision
The most common ask from operators right now is, “You’re already reading the referral packet. Can you do more with it?” The answer is increasingly yes. The next step for ExaCare AI is AI that takes the clinical and financial information it extracts at intake and routes it to downstream teams automatically.
The result: the data your intake team already captured at admission starts doing work downstream instead of sitting in one system while the rest of the building starts from scratch.
Real-time bed management and capacity planning
Connecting admissions intelligence with live census data is the next operational unlock. The question isn’t just “should we accept this patient?” It’s “where should we place them, given current occupancy, staffing levels, and clinical capabilities across the portfolio?”
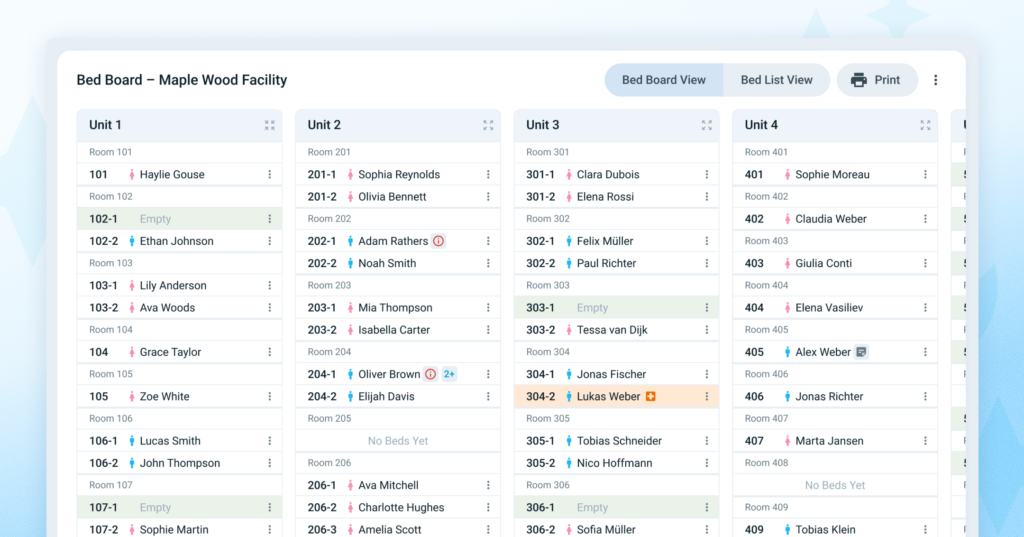
Bed board functionality that links directly to the admissions system is beginning to reach the market, giving operators real-time visibility into placement decisions they’ve historically managed with spreadsheets and phone calls.
Home health intake
The home health market faces the same fundamental referral management challenges as skilled nursing: manual review, fragmented portals, speed-to-respond pressure, with the added complexity of EHR integration hurdles.
Homecare Homebase (HCHB) dominates the home health EHR landscape the way PointClickCare dominates in skilled nursing. Like most deeply embedded EHR systems, HCHB integrations require careful coordination, which has meant AI adoption in home health has moved more slowly than in skilled nursing.
But the demand is clear: healthcare providers who can respond to referrals in minutes rather than hours win more patients. AI-powered intake is expanding into home health, and as integration coverage broadens, the impact should mirror what we’re already seeing in skilled nursing.
Predictive operational analytics
Operators who centralize their referral data now are quietly building something most of their competitors don’t have: a real picture of what’s coming next.
Not just what happened last quarter, but where census gaps are likely to open, which payer trends are accelerating, and which facilities are going to need support before the numbers show up in a monthly report. That capability isn’t widely available yet. But the operators who have structured data flowing through their intake today will be the first ones to use it.
How to evaluate AI for your post-acute organization
You probably don’t need convincing that AI is becoming table stakes for intake. The harder question is how to pick the right tool when every vendor’s demo looks impressive and you’ve seen enough CRM rollouts go sideways to know that what you’re shown in a sales cycle isn’t always what you get on the other side. Here’s what to look for:
- Start with your highest-volume bottleneck, not the most impressive demo: For most multi-facility SNFs, the answer is referral intake. That’s where the time savings are largest, the revenue impact is most direct, and the proof points are strongest. Resist the temptation to evaluate AI based on the most futuristic feature. Evaluate it based on what solves your most expensive problem today.
- Demand integration depth, not just feature breadth: AI that doesn’t connect to your existing referral portals, your EHR, and your team’s communication workflows creates another silo. Ask specifically, Which e-referral platforms do you integrate with? Which EHR systems? How do referrals get into the system… automatically, or does my team need to download and upload PDFs? If the answer is manual, the speed advantage disappears. Native EHR integration (whether that’s PointClickCare for SNFs or Homecare Homebase for home health agencies) is what determines whether you’re live in two weeks or stuck in a custom API project for three months.
- Look for real outcomes from real customers: Ask for case studies with numbers like time saved per referral, impact on referral volume, census changes, and revenue impact. Better yet, ask to talk directly to current customers. Any vendor confident in their outcomes should be willing to connect you with operators who are already live.
- Evaluate the implementation model, not just the software: Post-acute care teams have limited bandwidth for system changes. I’ve seen great software die on the vine because the implementation was a two-hour Zoom and a PDF. Your admissions team doesn’t have time to figure out a new system while processing 40 referrals a day. Ask how the vendor handles the first two weeks. That’s when you’ll know whether this is a partnership or a handoff.
Think about the data from day one: Most operators buy AI for the speed. But its value goes beyond productivity gains. When referrals and patient data live in email threads and PDFs that get reviewed once and filed, there’s no record of why you declined, how long you took to respond, or what your payer mix actually looks like across buildings. That data simply wasn’t captured. AI-powered intake creates it as a byproduct of doing the work. Six months in, that’s what really changes how you run the business.
The operators who move first will define the standard
The operators who’ve already adopted AI for intake aren’t wondering if it works anymore. They’re posting census numbers their competitors can’t explain. They’re responding to referrals in minutes while the facility down the road is still toggling between portals. Their leadership teams are making decisions with real data instead of reconstructing last quarter from memory.
Now, the operators who moved first are compounding their advantage every day: faster response times, stronger hospital relationships, better data, and teams that aren’t burning out.
Post-acute care has waited a long time for technology that actually fits how the work gets done. It’s here now, and the organizations adopting this infrastructure today are the ones who’ll be setting the standard everyone else has to meet.

